Thank fully, Australia seems to have turned a corner in the wake of the global pandemic. Nevertheless, news coverage of COVID-19 is constant, leaving little room to raise awareness about other issues affecting our community.
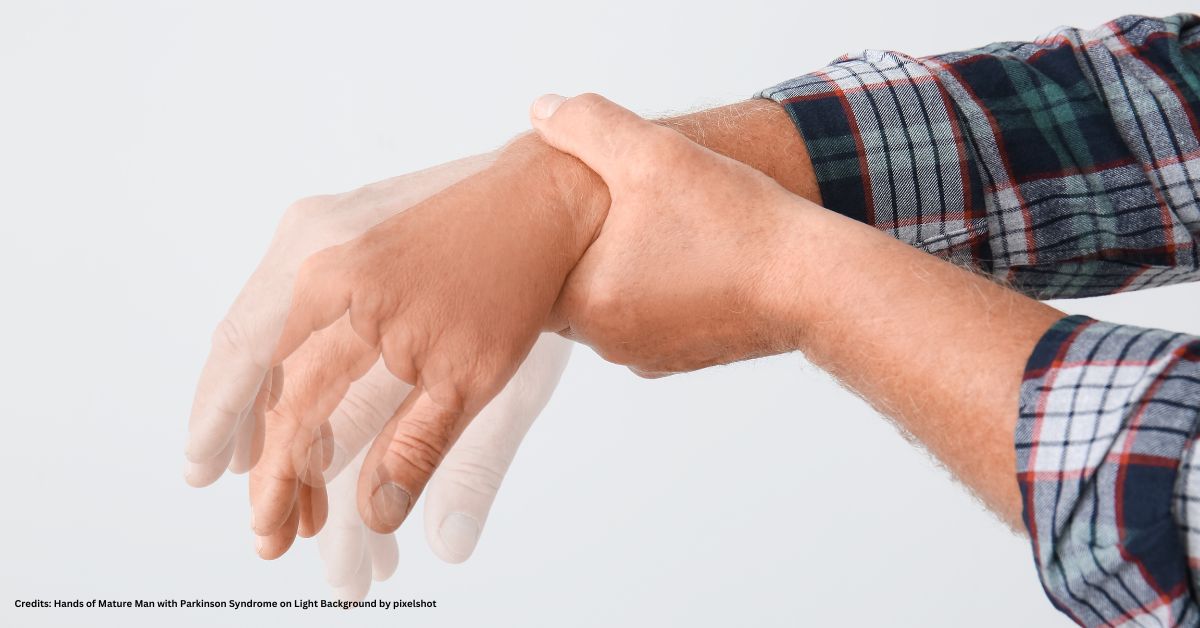
Cancer cases are still on the rise. In 2020, 147,956 cases of cancer are estimated to be diagnosed in Australia alone. Every one of those undergoing, or about to undergo treatment for cancer will be acutely aware of the increased threat they face from COVID-19.
Join Nikki’s 60-minute online seminar to learn how you can advance your fundraising strategies through the use of technology.
Many of us have rightly spent the past few weeks re-prioritising, focusing on family and friends who need us. If you’re able to, please consider including our cancer researchers and patients in this cohort. Their dependency on your generosity cannot be underestimated.
A promising project
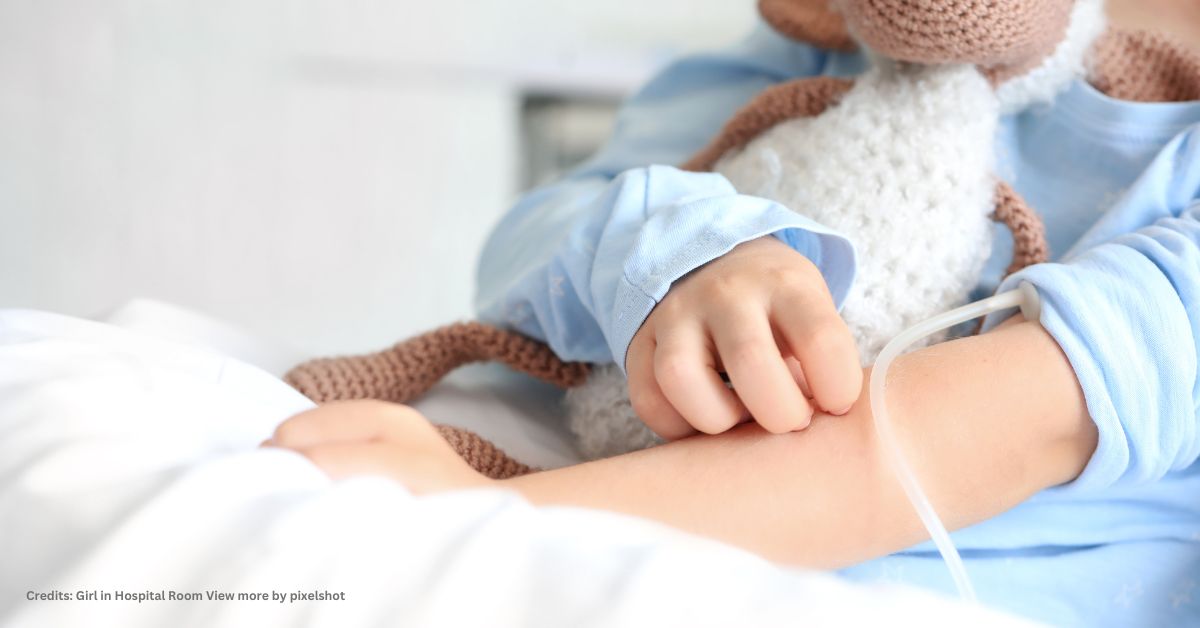
Dr Jessica Duarte is just one of the brilliant young scientists we’re working with this year. Based at the Olivia Newton-John Cancer Research Institute in Melbourne, Jessica’s project will predict treatment outcomes in rare cancers. Of the 147,956 Australians who will receive a cancer diagnosis this year, 42,000 of them will have a rare cancer, like childhood, brain, pancreatic, eye cancer, or one of the many others.
Despite 50% of cancer deaths being a result of rare cancers, they receive a mere fraction of the funding of more common cancers. Due to the lower incidence rate, rare cancers are often excluded from clinical trials and studies. While incidence is low for individual rare cancers, collectively they comprise almost 30% of all diagnoses.
Receiving a rare cancer diagnosis is incredibly distressing. Lower survival rates in comparison to more common cancer types are a major source of anxiety for patients and families. To further compound this, the increased dangers posed by COVID-19 will cause patients a huge amount of stress over the coming months.
Developing a personalised medicine approach
With the help of our supporters, Jessica’s study could lead to a personalised medicine approach where all cancer patients, irrespective of cancer type, have a unique treatment plan with a high likelihood of success.
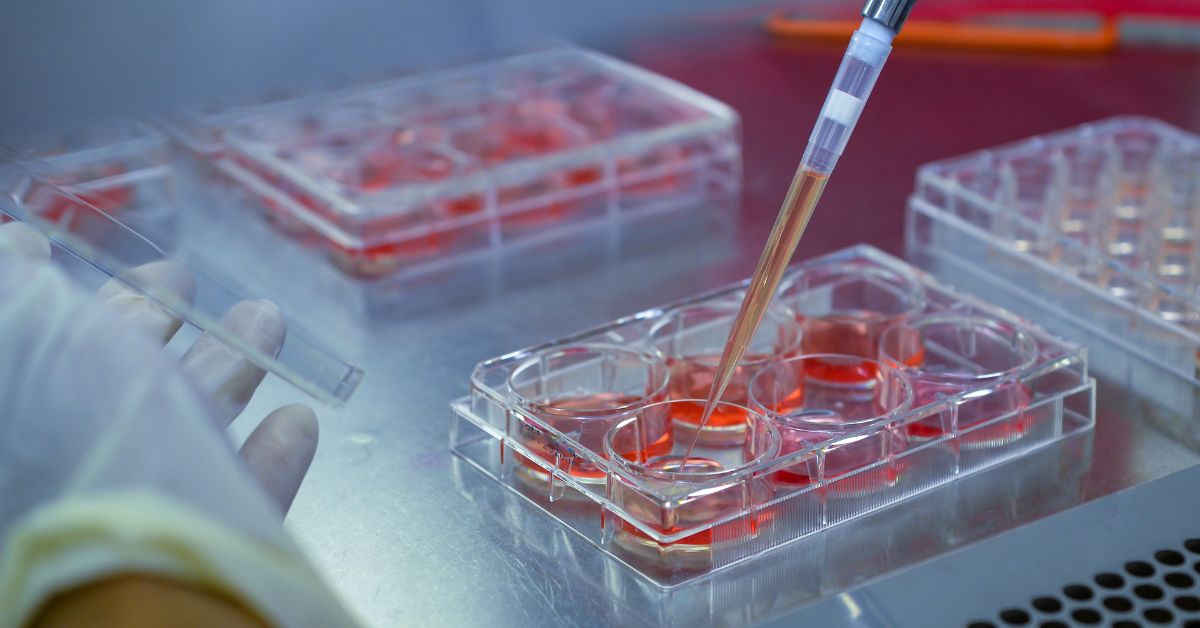
By analysing a drop of blood taken from patients undergoing immunotherapy, she aims to predict how they’ll respond to treatments aimed at boosting their immune systems.
“Effective immune engagement occurs when the immune system recognises and destroys a tumour cell,” Jessica explains, “but tumours have developed ways to escape this immune attack, which is when they grow uncontrollably. Patients who have strong immune engagement live longer.
“Our work may allow us to determine if a patient’s immune system is actively engaging with the tumour, and thereby predict their likelihood of responding well to immunotherapy treatment.”
Research is our only hope of making this the last generation to die from cancer.
We can’t afford not to try.